This modpack is currently disabled.
Install Influence of Nurse Practiс
Step 1
Installing a modpack using the Technic Launcher is easy. If you don't already have the launcher downloaded, visit our download page to get the latest version.
Step 2
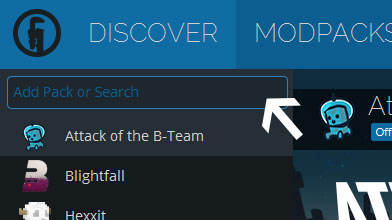
Type in the modpack name (Influence of Nurse Practiс) or paste the following url into the search box.
Step 3
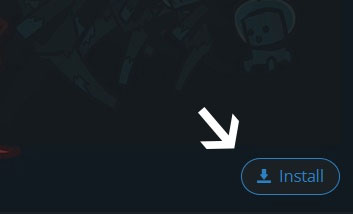
Finally, click Install at the bottom right of the launcher after you select Influence of Nurse Practiс from the list on the left. The launcher will handle everything else!